Turbinate reduction, sometimes known as turbinate surgery or turbinoplasty, is a procedure used to reduce the size of the inferior nasal turbinates which are responsible for nasal congestion. This action provides for improved airflow through the nasal cavities. Typically, the procedure takes place through the nostrils on both sides of the nose. This procedure is often performed in the office under local anesthesia as a stand-alone procedure or in combination with balloon sinuplasty. It can also be performed in an outpatient surgical setting with the patient under general anesthesia in combination with other procedures like septoplasty, vestibular stenosis (aka nasal valve repair) and /or endoscopic sinus surgery.
 When are Turbinate Surgeries Considered?
When are Turbinate Surgeries Considered?
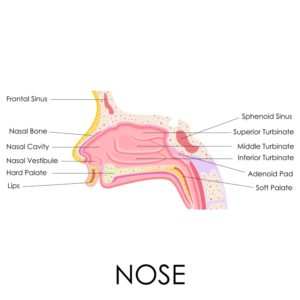
There are three turbinates on each side of the nose. They are:
- The inferior
- The middle
- The superior
The turbinates’ job is to filter and humidify the air we breathe in as it moves from the nose to the lungs.
Some individuals, however, have what is called turbinate hypertrophy, the nasal obstruction explained above. Various procedures are used to reduce the size of the turbinates in the nose. They serve to lessen resistance in a patient’s airways while the essential functions of turbinates remain in place. The procedures aim to improve breathing through the nose, as well as decrease nasal drainage, and postnasal drip. Allergies, environmental irritants, smoking, infection as well as other factors including pregnancy can contribute to turbinate hypertrophy.
When treatments like nasal steroids, nasal rinses, antihistamines, and decongestants do not eliminate sinus problems, permanent minimally invasive surgical procedure are available.
Types of Turbinate Reduction Procedures
Nasal turbinates are essential for normal nasal respiratory function such as air humification and air filtration, thus surgical procedures aim to reduce the blockage of air flow without altering the mucosal lining of the turbinates. The types of procedures performed in the community can include:
- Turbinectomy (partial removal of the turbinate – fraught with complications)
- Turbinate cauterization (burning the turbinate – can affect the turbinates humidification and filtration abilities)
- Coblation of the turbinates (cold laser reduction – nice technique but often the hypertrophy or inflammation recurs and has to be repeated often)
- Submucous resection of the turbinates – SMR (Dr. Cohen’s preferred technique and main technique recommended by most Nose & Sinus Specialists as well as the American Rhinologic Society as well as the American Academy of Otolaryngology – Head and Neck Surgery)
Anesthesia for SMR turbinates:
Often performed under local anesthesia in the office as a standalone procedure or in combination with Balloon Sinuplasty. Also often performed in combination with septoplasty, endoscopic sinus surgery and/or nasal valve repair in an outpatient operating room setting with the patient under general anesthesia. Both settings provide equivalent results, however Dr. Cohen tailors the procedures for each patient according to their particular issues and concerns and what would be best and safest for each patient.
Complications of SMR turbinates:
As with any procedure the risks can include pain, bleeding, infection, scar tissue formation or recurrence of the problem needing the procedure to be repeated. These risks are seen in less than 1% of cases done by Dr. Alen Cohen.
Post-procedure care after SMR turbinates:
Often after the procedure there is mild to moderate scabbing and crusting along the nasal passages that takes about a week to resolve with sinus rinses. During this time the patient feels mildly congested like having a cold but as the scabs resolve, the patient will start to feel tremendous improvement in their breathing and congestion. Patients often return to work in 1-2 days, if this procedure is done as a stand-alone procedure in the office under local anesthesia. Nonetheless, this procedure is often combined with in-office Balloon Sinuplasty in Dr. Cohen’s hands.
Balloon-Sinuplasty
Dr. Cohen is the Director and Founder of the Southern California Sinus Institute, which is Los Angeles’ premier sinus center for In-Office Balloon Sinuplasty and Turbinate Reduction. As such it has been recognized as a Nationwide Sinus Center of Excellence. He uses these procedures to help patients with the following medical issues:
- Enlarged turbinates
- Environmental allergies resistant to medical therapy
- Nasal obstruction/congestion
- Deviated septums
- Nose and sinus polyps
- Acute and chronic sinusitis
- Recurrent sinus infections
- Sinus headaches
- Snoring and sleep disturbance
- Smell and taste issues
- Chronic postnasal drip and cough
Dr. Cohen’s In-Office Balloon Sinuplasty
Dr. Cohen’s appreciation of this in-office procedure is because of several factors but primarily because it is minimally invasive, low cost, minimal discomfort, minimal downtime and has permanent results.
The procedure treats many conditions and irregularities that include:
- Inflammation of the paranasal sinuses
- Acute and Chronic Sinusitis
- Recurrent sinus infections
- Sinus headaches and pressure
- Environmental allergies refractory to medical management
- Nasal polyps
- Chronic infection (bacterial or fungal)
- Chronic nasal obstruction
- Deviated septum
- Enlarged turbinates
- Facial and sinus pain
- Constant runny nose
- Postnasal drip
- Chronic cough
- Recurrent ear and eye infections
- Ear congestion
- Ear fullness
- Even tooth pain
The Southern California Sinus Institute performs balloon sinuplasty in their Los Angeles area offices. The procedure consists of expanding nose and sinus pathways by reshaping the anatomy of the nose permanently. As a result, the restoration of normal breathing and proper drainage of the sinuses occurs.
The Procedure
Dr. Cohen begins by topically numbing the nasal passages and sinuses with various ointments, sprays and liquid-filled cotton balls over 20 minutes. No needles are used at all during this initial numbing process. Once adequately numbed the sinuplasty procedure begins with placing tiny balloons into the sinus drainage openings and inflating them for a few seconds to expand the sinus pathways and then removing the balloons. The balloons cause microfractures of the sinus openings and permanently change the openings of the sinuses so they can drain better and more properly. This procedure permanently restores normal drainage patterns for the sinuses thus reducing the frequency and severity of sinus infections as well as minimizing sinus headaches and pressure.
Dr. Cohen’s technique does not require general anesthesia. The treatment takes place in the doctor’s office under local anesthesia by way of topical medications. The procedure itself only takes 20 minutes but the numbing process also takes about 20 minutes. There is practically minimal recovery time needed after the procedure. Patients are usually back at work within the next 24 to 48 hours.

- Instant relief of sinus pressure and pain
- Reduction in the number of sinus infections
- Lowered medical bills as prescriptions and office visits concerning your sinuses lessen
- Improved breathing
- Improved sleep
- Decreased snoring
- Improved quality of life
- Less disruption to daily activities
- Minimal discomfort or pain
- Permanent results
This revolutionary in-office sinuplasty is often combined with turbinate reduction so as to address nasal congestion and breathing problems for patients at the same time. Dr. Cohen and his ENT team can assist you in making the right decision as to which procedure would best serve you.
Most PPO insurances and Medicare prefer this procedure over more invasive sinus surgeries that take place in an operating room due to lower costs and decreased risks associated with the procedure.
Contact our offices today and let SoCal Sinus get you onto the road to better health and a better life.

